
MEDIA RELEASE
3 July 2024
First Nations children aged under two at greater risk of ear disease-
but headway is being made, new data shows
Regular checks are critical to address the issue, urges Hearing Australia
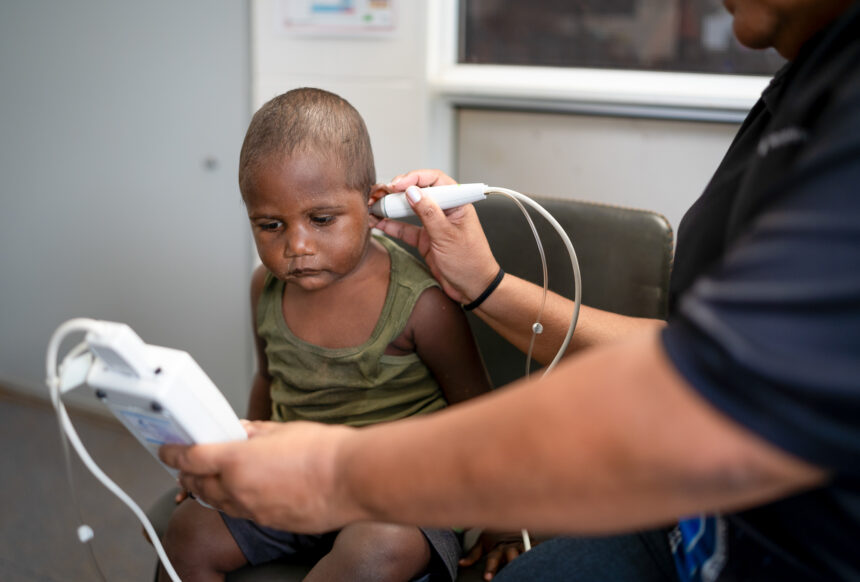
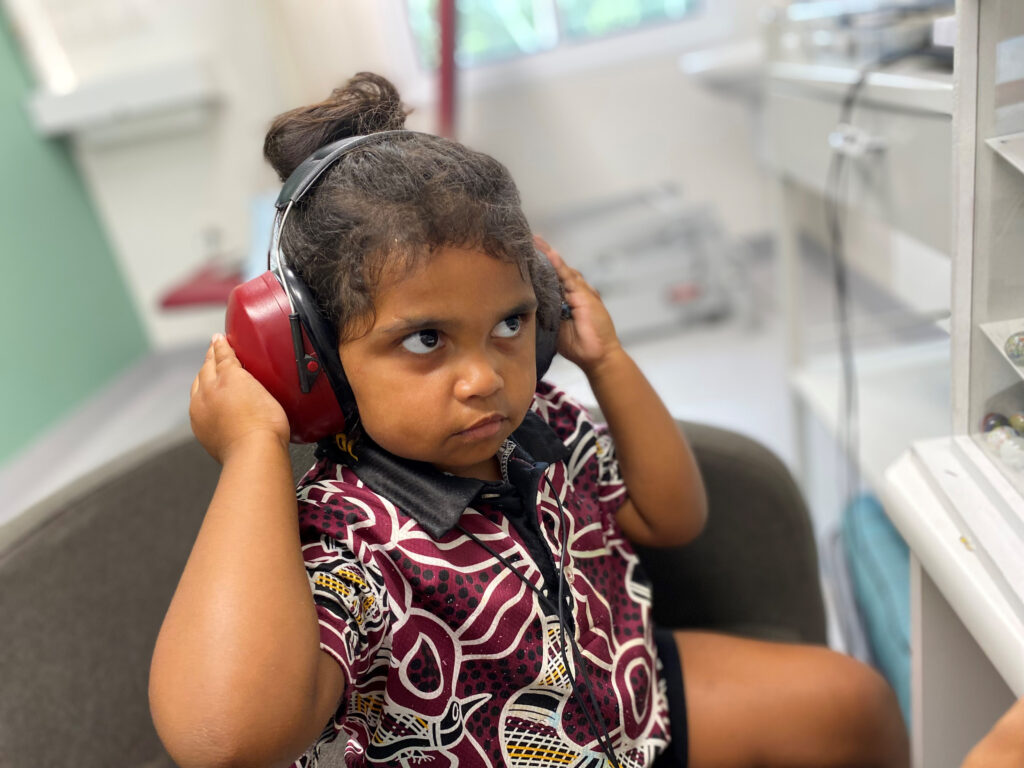
Middle ear infection (otitis media) in Aboriginal and Torres Strait Islander children remains among the highest globally1. And those aged under two have a much higher risk of undiagnosed ear disease, new Hearing Australia clinical findings2 show. As NAIDOC Week kicks off (Sunday July 7), Hearing Australia is encouraging parents and primary healthcare providers to make sure young First Nations children have their ear health checked as often as possible.
As part of its HAPEE program (the Hearing Assessment Program – Early Ears), Hearing Australia recently analysed the hearing assessments of 19,000 First Nations children across the country, with some alarming findings:
- More than 26 per cent of children assessed were found to have undiagnosed ear disease and one-in-five had undiagnosed hearing loss.
- Children under two have more ear trouble than older children, and those in very remote locations have more problems than children in regional or metro areas.
There is overwhelming evidence that hearing loss in young children can impact their learning and development3. “However, the good news is we are making headway in seeing children and getting them the help they need,” says Yorta Yorta woman Kirralee Cross, from Hearing Australia’s First Nations Services Unit. “In 2022-23, we assessed 14,435 First Nations children, the most in any year since the HAPEE program began in 2019. The data also shows that, while some 60 per cent of children have better hearing health when seen at a follow-up appointment, more needs to be done to improve community awareness of the importance of ear and hearing health.”
Kirralee says there needs to be a paradigm shift to tackle otitis media among First Nations children. “Ear infections are common in children but for First Nations children they typically occur more often, start very early in life and last longer”, she says. “There’s an urgent need for action at many levels – from the health system, service providers, practitioners, and parents/caregivers. First Nations cultures are traditionally shared through language, dance, song and art. So, not only do we need to ensure our children can hear well to learn, but we also need our children to hear well to learn the stories being passed down by Elders to help keep our culture alive.”
Kirralee urges parents to “speak up” if they have any concerns and to get their children’s hearing checked regularly – even if there are no obvious signs of problems. “Middle ear disease can be difficult to detect; there may be no symptoms like earache or fever. Which is why we also urge primary healthcare providers to assess ear health early, effectively, and regularly, to identify First Nations children with persistent problems, and get appropriate treatment and support in place,” she says.
Six-monthly checks recommended
A recently published paper,4 released new evidence and consensus-based recommendations for routine Ear Health and Hearing Checks (EHHCs) for Aboriginal and Torres Strait Islander children aged under six years. The recommendations, for primary health practitioners, are six monthly EHHCs until the age of four and then one check at five years of age. They also suggest4 that checks be conducted more frequently in high-risk settings and for children under two.
The paper references the Otitis Media Guidelines for Aboriginal and Torres Strait Islander Children5, which advocate that ear health checks happen for Aboriginal and Torres Strait Islander children during every primary healthcare visit. However, in previous research, parents, caregivers and health practitioners reported that this hasn’t been happening. Instead, checks are most likely to happen when parents or caregivers request them – which is not an easy ask – when signs aren’t obvious.
Simple but powerful part of the toolkit to detect ear health issues
The Ear Health and Hearing Check recommendations include the routine use of tympanometry, which reveals how well the middle ear is working and provides a quick and easy indication if there’s an ear health problem. “Our data2 shows that children who fail tympanometry tests have a much higher likelihood of hearing loss,” explains Kirralee. “This test takes around a minute to do. It’s an excellent way to detect ear health problems. To enable the routine use of tympanometry, Hearing Australia offers training and support to primary healthcare providers.”
Mr Kim Terrell, Hearing Australia’s Managing Director, says the HAPEE program, which is delivered in close partnership with multiple Aboriginal Community Controlled Health Organisations and local communities, is crucial to improving the hearing health of First Nations children and building the capabilities of primary health services.
“We are fortunate to work with many amazing partners and we acknowledge their commitment to helping prevent avoidable hearing loss in First Nations children,” says Kim. “Checking the ear and hearing health of young children is a critical step to preventing long-term ear disease and hearing loss. With the support of government and our many partners, we will continue to listen to First Nations peoples and work closely with communities and local services to improve the ear and hearing health of individuals and families.”
ENDS
Disclaimer
The Hearing Assessment Program is an initiative of Hearing Australia and funded by the Australian Government. Aboriginal and Torres Strait Islander children not yet attending full time school are eligible to be seen. All services provided under this program are free of charge. A hearing check includes a number of age-appropriate tests of hearing and middle ear function.
Conditions apply under the Australian Government Hearing Services Program
References:
1. World Health Organization. World report on hearing. Geneva: World Health Organization, 2021. https://www.who.int/publications/i/item/9789240020481 (viewed June 2021)
2. Based on data collected under the HAPEE Program
3. Tomblin, J. B., Harrison, M., Ambrose, S. E., Walker, E. A., Oleson, J. J. & Moeller, M. P. 2015. Language Outcomes in Young Children with Mild to Severe Hearing Loss. Ear Hear.,36 Suppl 1, 76S-91S.; Ching, T. Y. & Dillon, H. 2013. Major findings of the LOCHI study on children at 3 years of age and implications for audiological management. Int. J. Audiol., 52 Suppl 2,S65-8
4. S Harkus, V Marnane, I O'Keeffe, C Kung, M Ward, N Orr, J Skinner, K Kong, L Fonua, M Kennedy and M Belfrage, Med J Aust 2023; 219 (8): 386-392. || doi: 10.5694/mja2.52100. Available from Routine ear health and hearing checks for Aboriginal and Torres Strait Islander children aged under 6 years attending primary care: a national consensus statement.
5. Menzies School of Health Research. Otitis Media Guidelines for Aboriginal and Torres Strait Islander Children Darwin: Menzies School of Health Research; 2020 [cited 2021 June 16]. 3:[Available from: https://www.menzies.edu.au/icms_docs/324012_Otitis_Media_Guidelines_2020.pdf.
About us:
About Hearing Australia
Hearing Australia has provided expert hearing care to Australians for over 75 years, helping thousands of children, adults, Aboriginal and Torres Strait Islander peoples, pensioners and veterans stay connected with their families and communities every week. Now, more than ever, good hearing is important to keep in touch with loved ones and stay connected to the world around you. With more than 450 audiologists, we offer services through tele-services, online, in home and in centre across over 450 locations Australia-wide. Our goal is to keep you connected to the people and life you love. No matter your age, no matter your hearing need, we make hearing easier for everyone.
Contact details:
Llewellyn Communications
Lisa Llewellyn
0419 401 362
Hearing Australia
Melanie Berenger
Melanie.Berenger@hearing.com.au
0414 607 581