
Scientists have uncovered an important new link between the brain and immune system after stroke, which could lead to potential new treatments to improve recovery and reduce long-term disability.
In new research published in international journal Frontiers in Immunology, researchers from La Trobe University and the Baker Heart and Diabetes Institute discovered that the spleen actively produces inflammatory immune cells after stroke that can worsen brain injury.
By blocking a key inflammatory signal called S100A8/A9 in experimental models, scientists reduced brain damage by around one-third and improved recovery.
Stroke is a leading cause of death and long‑term disability worldwide. While current treatments focus on restoring blood flow to the brain, which is still critical, they do not address the damaging inflammation that continues after the initial blockage is cleared.
This research suggests a completely new way to aid recovery and reduce long-term disability after stroke, by targeting inflammation.
“Inflammation can cause ongoing injury to the brain, even after blood flow is restored,” said La Trobe University research lead Dr Helena Kim.
“Our findings show there may be new ways to limit this damage by targeting the body’s immune response. This is an early but exciting step in better treatments for stroke patients.”
S100A8/A9 is a protein signal released by immune cells during inflammation. After stroke, it appears to act like an alarm signal that tells the body to produce more inflammatory cells.
While this response is meant to help fight injury, in stroke it can make things worse by increasing swelling and damaging brain tissue.
To test whether this immune overreaction could be controlled, the researchers used a drug that blocked the activity of S100A8/A9.
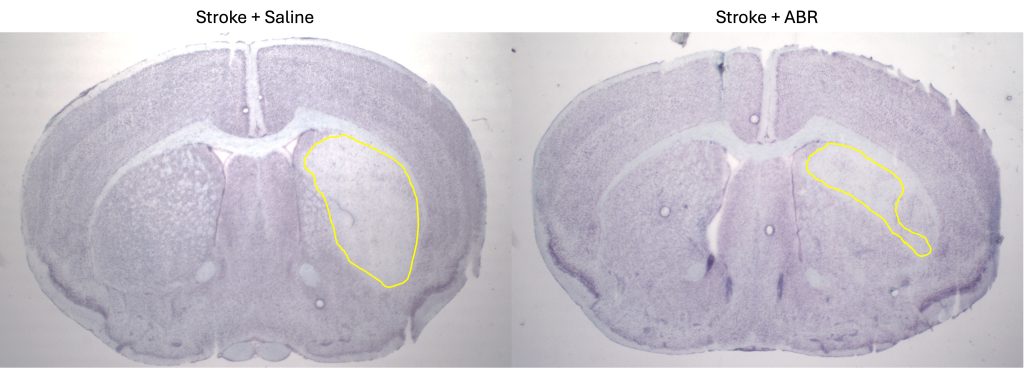
Animal models treated with the drug before and after stroke had far fewer inflammatory immune cells produced in the spleen, lower numbers of these cells circulating in the blood, about 35 per cent reduction in brain damage and better physical function within 24 hours.
“When we blocked this signal in a pre-clinical stroke model, we saw fewer harmful immune cells being generated, smaller areas of brain damage and better neurological recovery,” said Dr Sam Lee, the senior scientist of the study from the Baker Heart and Diabetes Institute.
“We discovered that the majority of these inflammatory immune cells actually come from the spleen. This helps explain why inflammation becomes so widespread in the body after stroke and highlights the spleen as an important new therapeutic target.”
The team also examined brain tissue from people who had experienced severe strokes and found the same inflammatory signal present in damaged areas, supporting the relevance of the findings to human disease.
The results suggest that targeting inflammation – particularly signals that drive harmful immune cell production – could complement existing stroke treatments.
“Rather than wiping out immune cells altogether, which can be dangerous, this approach aims to switch off the signals that cause excessive and damaging inflammation,” Dr Kim said.
Further studies are needed to confirm effectiveness across different patient groups but Dr Kim said the discovery could potentially lead to improved treatments for other conditions with the same inflammatory pathway including heart attacks and other vascular diseases.
Media enquiries
Charisse Ede – media@latrobe.edu.au, 0404 030 698


